We start at 6:30 a.m. and the first thing I check is the assignment board, to see what kinds of patients are scheduled. Chest pain. Clogged arteries. Various arrhythmias. Shortness of breath. And there's always the chance of an emergency wheeled in on short notice to spice things up.
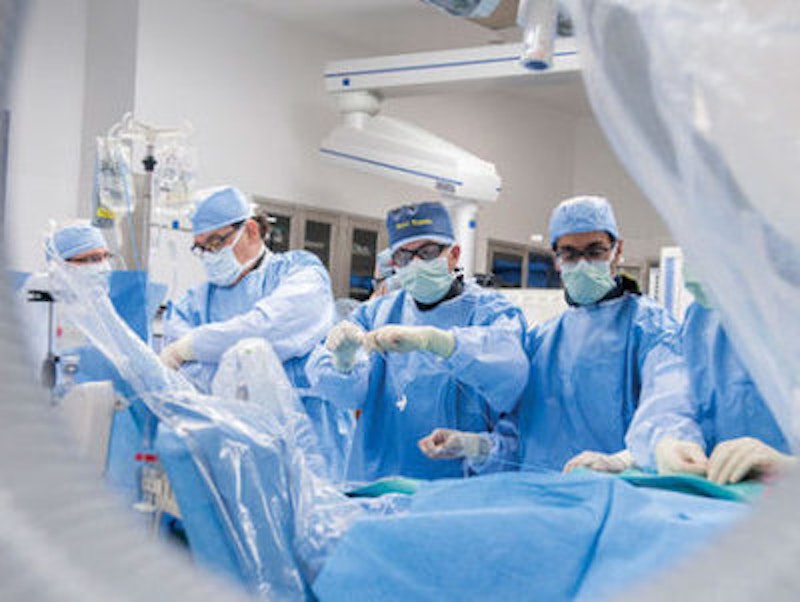
The cath lab at the Miracle Center takes up an entire floor. There are seven rooms, each with a doctor and a team of four techs. One room is devoted to the electrical system that governs the heartbeat. This is electrophysiology, and the room is unpopular with the techs: steep learning curve, dense material, not much action. The other rooms quantify the heart’s function as a pump: leaky valves, clogged arteries, septal defects. We don’t do surgery here; valve replacements and transplants and bypass operations happen downstairs.
I’m scrubbed in, and keeping the field sterile is my main concern. This includes me, from my elbows down to my hands, and from my waist to my chin. The only sterile area in the room itself is the space in the immediate vicinity of the patient's torso. Sterile is an approach, an intention imposed upon a limited physical space by the strict regulation of physical behavior; it’s a location within a room, but could never be the entire room. There was a time when sterile didn't exist, when doctors operated in top hats and greatcoats, without masks, gloves, or even hand-washing. Today, if I find even one stray hair, the whole table is scrapped as contaminated.
One thing that drew me here is the idea of actual fixing. Somebody comes in with a problem; we give them a stent or a valve or a pacer, and they go home. It’s not like Parkinson’s or diabetes or Alzheimer’s, which I see as death on the installment plan. Cancer interests me on the cellular and genetic level, but it’s sort of like rust; you can’t tell if you “got it all” and it could reappear down the road. I like seeing an immediate result.
My tasks as scrub are to prep and drape the patient; mind the sterile field; check that everything I might need is at hand; and anticipate the cardiologist’s next immediate need. I always talk to the patients, try to reassure them. “This is a procedure, not an operation,” I explain. “You'll only be mildly sedated, and can watch on the screen if you like.” A lot of them don’t want to watch, for obvious reasons. Too close to gore and death. I understand and don't understand at the same time, because I was a watcher when my turn came. Once in a while we'll get patients who asks a million questions and can't take their eyes off the monitors. These are the ones I encourage to ask questions, to describe their pasts. In rare cases, they’ll talk about a past surgery or other close calls. If I detect absolute interest, I might indicate the scar down the middle of my chest.
Our first patient, a late-middle-age woman, is not a watcher; she wants out as quickly as possible. She wants to be home. Today's events will not change one aspect of her daily routine. With a lot of customers, you can just tell; it's the way they answer questions with the minimum number of syllables, look around as if being here was an inconvenience or an intrusion. Our lady lies on the narrow table; she is fairly obese. More chins than the Hong Kong phonebook. The table is rated for 200 kilos. It took several of us to get her up there. We secured her panniculus to the sides of the table with packing tape to expose her groin to daylight; she apologized with some embarrassment for not being able to wash all of herself.
I feel around the groin for the femoral artery, but it's hard to locate a pulse underneath all her flesh. I place the cut-out in the drape over the general area. I create little pouches with sterile towels and clips, to hold wires, syringes, and hardware; the patient's belly becomes my workbench. Syringes are filled with lidocaine, catheters are flushed with saline, instruments are aligned in approximate order of need. Sterile packages are opened by the room circulator, contents spilled neatly on the back table. There’s lots of stuff at my disposal; it’s a CSI lab for the heart. I’ve always been mechanically inclined. We grew up poor, and I learned early on to fix my own bicycles and roller skates. The cath lab for me is like a playroom, or a tool shed. I check the overhead monitors, but we haven't placed any catheters yet, so all that's showing is her EKG, from the tabs we placed on her skin. Now comes the fun part. The cardiologist probes with a fat hollow needle, finds the artery; a jet of quick red blood surges thinly. This is the Seldinger technique, what we call the stick. A short wire goes in through the needle, and the needle comes out over the wire. Flush the needle; wipe down the wire that’s now sticking out of her like excess guitar string off the tuning peg. Now a 6-French sheath goes in over the wire, and the wire comes out; save wire to saline bowl, just in case. It's all very slick. In just a few seconds we have created a portal with which to access the interior of the heart. Through this sheath we can put wires, balloons, stents, drill bits, catheters for injecting dye and taking internal pressures. A German med student named Forssmann was the first person to access the heart's interior; he did it to himself, with a urinary catheter, in 1929. A fellow student x-rayed him and located the catheter tip in the right atrium.
With a catheter now in place the patient's blood pressure suddenly appears on one of the monitors. But they are more than numbers now; there's a waveform rolling across the screen, and every notch and slope and peak and valley in the wave means something. This is the physical shape of the systolic and diastolic pressures changing over time. The waveforms are speeding by at almost two per second. The cardiologist reads with no words, like a conductor reading a score, hearing music in his head. Evaluating heart function.
I watch the EKG screen, another pattern of waves, but limited to purely electrical activity. The heart is driven by electricity, and excess current leaks through to the surface of the chest and is recorded on pink graph paper. Every segment of the wave describes the movement of a tiny chunk of heart muscle. How did such a machine come about?
•••
I should explain how I got here. My mother’s parents died on the same night in 1946, three hours apart, of separate heart diseases. My mother died of a ruptured aorta. My father died after three heart attacks. One of my brothers dissected his aorta. One of my sisters dissected some coronary arteries. We share a connective tissue disorder driven by a gene, FBN1, on chromosome 15. The bottom line of this disorder is that the aorta never stops growing in diameter, so the walls thin out, weaken, and split apart. I inherited this gene from my mother.
They kept an eye on me for many years, and replaced my aorta and aortic valve before they blew. I’ve had CT scans, echocardiograms, MRI, gamma camera. The imaging technology killed me. I was a watcher when they sent me to the cath lab for my pre-op catheterization. I watched the screens, I asked questions. Sure, I was on some drugs, but still. I was flabbergasted by the pictures of my coronary arteries, and the last question I remember asking was, what kind of schooling do I need to have this job? I went back to college at 50 and studied cardiac anatomy and physiology for two years.
•••
Back to the woman on my table. Only the x-ray monitor shows anything even remotely recognizable as human: some spine and ribs, the dark disk of the diaphragm. Loops of piano wire where her sternum was yanked back together after a previous surgery. Tiny perfect circles where none should exist; she's been bypassed, and those are the graft markers.
Being there, inside her heart with the catheters, fascinates me; even if we cut her heart open and examined it with a magnifying glass, we would not learn as much, could never see the history available on the screens. Integrate the EKG readings with the insane hieroglyphics of the pressure tracings, the bracketed numbers and pulsating stars on the computers, and you have a real-time video of the heart in action. I'll be dead long before I can ever become bored.
We have injected contrast dye in both coronary branches and taken our pictures. One of the body's finer miracles is revealed immediately: collateral vessels growing where she began to sprout new circulation around the blockages. This woman has several issues. There's a build-up of calcium on her aortic valve leaflets; there are several lesions that will require ballooning; and there's a part of her left ventricle that remains immobile while the rest pumps weakly. A graft has re-closed. Why do I think of her as a project, rather than a person? We are a system composed of numerous sub-systems, each sending signals to the others with inconceivable rapidity. An infinity of cellular and molecular call-and-responses. I'm very good with the patients beforehand and afterwards, reassuring them, answering and asking questions, explaining what I can. But while they are sedated and we are working, I can't help myself. It never fails: the more disease the patient comes in with, the better I feel.
We balloon the plaque against the walls of the LAD, the left anterior descending coronary artery, packing it like oatmeal. That's part of the job I like, pumping up the balloon, watching it move along under the cardiologist's guidance, inflating some more: so many atmospheres for so many seconds. It's almost impossible to believe there's a living person at the distal end of the balloon. Now we can stent the artery to hold it open. From my position as scrub, the patient's fate is in the hands of the other techs in the room. They have to follow the screens, inject the drugs, defibrillate with the paddles if she goes into ventricular fibrillation, make room reservations in the OR if needed. My job is to assist Dr. J, whose actions, like mine, are limited by the demands of sterility. The proper time for questions comes at the end of the case, when we can read the pictures and patient history more thoroughly, but this doesn't prevent me from expending enormous energy trying to understand the case in real time.
I remind myself that this woman is a person with a family waiting a few rooms over. If she dies, the family will believe that modern medicine has failed them; the doctor might believe he made some miscalculation; the larger medical community might look for a pattern or process that might be avoided next time; catheterization protocols could be changed. Her case, if extremely unusual, could get written up in a journal. But, I tell myself, she, up in heaven, will simply recognize that her time had come. If I saw things any differently, I couldn't do my job.
There’s an unspoken assumption here at the Miracle Center, probably at all hospitals, that we are here to save lives, and we are. But once you’ve worked here, seen the people come in the doors in every conceivable state of poor health, reality takes hold. As in the outside world, people die here every day, people so ill that even God can't save them. We can't extend lives indefinitely, so what's our real purpose? I hope we alleviate suffering and add a few decent years of life. But everyone on the floor has seen patients die, and I quickly learned that, in the larger scheme of things, it’s neither good nor bad: it just is. And if watching death and thinking about death scares any of the techs, I haven't seen it. There is very little talk about patient suffering, mortality, life after death, or ethics. Meanwhile, even the patients who do die enter the record books; their facts and medical histories are documented and commented upon; those documents enter the literature, and medicine, with every case. There are questions when they live, and different questions when they die. For me, even a dead patient is a learning experience. I'll be one myself some day.
•••
An emergency AMI is wheeled in to the next room, a con from the prison up in Thomaston. My first thought is that he has better medical coverage than me. He’s escorted by two armed guards, as if he might try to make a run for it, heart attack and all. It seems incongruous, guns in the cath lab. All the loose techs and a few of the docs crowd the room or peer through the plate glass window. It happens with every emergency. A human fascination with heroics and death, bets on the outcome, apprehension. Add some sex, and we could be on reality TV. When you work here long enough, emergencies are all that matter. Even the dead come to life for an AMI. After the case, the doctor will take some time to explain the chain of events that caused the heart to stop.
Finally we're done with our patient; we’ve re-opened the graft and two blocked arteries. We bring her to the recovery room so I can hold healing pressure on the arterial puncture site. I don't understand why we don't use a fiber plug to seal the hole, at least on the obese. Probably the expense; we’re paid so little that it's essentially free to hold pressure for 20 minutes, while the plug is hundreds of dollars. I'm daydreaming, wondering how long it will be before this lab becomes obsolete; wondering what those in the future will think when they cut this lady open and find her arteries jacked open with pen springs.
Monitor, monitor. My lady's femoral pulse isn't so great, and I can't feel any pulse in her foot, so have no way of knowing if I'm occluding the access artery properly. I wish she were thinner, so her pulse would jump. But she is responsive, her monitor signs are good, color is good, and she's conversant. She's not chipper but she's talking. I wish I liked her, cared about her more. Oxygen saturation 93 percent, heart-rate okay, textbook EKG. Monitor the patient, not the monitor. Half an hour later I send her back up to her room.
•••
Later that afternoon, a bad thing happens. My buddy Poolboy interrupts my lunchtime. "Z, better get back to your room." An ugly surprise awaits me as they wheel my morning's fat lady back into the lab. Different room, different doctor, but this constitutes an emergency, a woman on the verge, and the room fills with drifters accordingly. Her blood pressure’s dropping like a dead guy, her skin looks like cement. She looks lousy, much worse than when I left her. All kinds of dosage calculations are flying around the room as the doctor tries atropine, dopamine, levophed, different drugs to raise the blood pressure, boost the firing of the SA node, increase the conductivity of the AV node, anything to jump-start her heart. Her pulse is nowhere. It occurs to me that she has bled out internally, that I failed to seal the access artery. If so, she's finished: there's no blood left in the vasculature with which to generate blood pressure. I eye the Zoll paddles as she slips in to cardiac arrest. "CLEAR!" I give her the paddles to the chest, and her whole body jumps off the table. She comes back for a moment and my apprehension abates, but she slips again and I shock her again but she fails for good. There's my flatline. We've been about it for an hour. "Let her go," the doctor says. It's the first time I've heard it put that way. Let her go, life and death, just like that. A decision.
We clean up the room a bit so the family can come in. Now I begin to defend myself. Why can't we plug the fat ones instead of holding pressure? Was the initial stick too high? But soon, direct questions come to me, from myself. Why am I not scared or depressed? Is it too soon to have an emotional reaction? I felt worse cutting EKG tabs in half so I could fit them all on an infant’s chest.
Nobody chastises me. One of the other doctors questions the original Seldinger stick. Was it a poor stick, the arterial access site too high up the artery for a proper hold? Can I cling to that, like the fifth shooter firing a blank during an execution? (The stick wants to be right above the ball-and-socket joint so you can hold arterial pressure against the bone.) Death comes, but the team supports the effort, not the outcome. We know the same things, that the people who come to the cath lab are sick; the procedure is not riskless; this is not an exact science. Wires break inside people; balloons refuse to deflate; plaques break off and race downstream; patients react unexpectedly to medications. Still, a tech needs to believe that death is reserved for doctors.
My questions start to pile up. Did I not hold long enough or heavily enough to seal the artery? Had I missed physical signs of her impending failure while holding? Did she have co-morbidities, those other health issues negatively affecting her chances? It doesn't matter; I’ve materially participated in someone's death, and all the physiology and chemistry bullshit I tell myself is up for review. I am responsible for something, but I just don’t know what it is.
Poolboy throws an arm around me, says let's go out for some pops.